6 Arterial blood pressure – measured invasively or non-invasively – and heart rate are also monitored throughout the test. When measuring CO during exercise, we choose from the thermodilution technique and the direct Fick method, which have both been validated for this purpose and the choice is made by considering operator expertise, exercise protocol in use and equipment availability. We also use the average pressure measurements from >2 respiratory cycles in preference to end-expiratory measurements. 
4,5 Our laboratory uses a submaximal exercise protocol to mitigate interferences in haemodynamic waveforms caused by large respiratory swings. 4 Since vascular tone and preload conditions change when the upright/semi-upright position is adopted, we suggest that right atrium, pulmonary artery pressures and pulmonary artery wedge pressures (PAWP) and cardiac output (CO) are recorded in the upright/semi-upright position before exercise, and the measurement is performed in the same way at rest as they are during exercise. After supine right heart catheterisation, patients are transferred to the cycle ergometer and pressure transducers are zeroed at the mid-axillary level. 2,3 In our centre, we have adopted the semi-upright position (30–45º head-up tilt), using a reclining table-cycle ergometer. Supine exercise using a table-mounted ergometer is easy to use, particularly for severely compromised patients but limits ambulatory activity, whereas upright or semi-upright positions avoid this but require the patient to be transferred from the catheterisation table. Heterogeneous procedural practices are encountered for the performance of exercise after initial right heart catheterisation. Once vascular venous access is secured, a balloon-tipped fluid-filled catheter is positioned in the pulmonary artery under fluoroscopic guidance and diagnostic right heart catheterisation is performed at rest. Since the majority of complications of right heart catheterisations are related to vascular access, our institution has chosen ultrasound-guided upper extremity venous access as our standard vascular venous access site so we can mitigate those risks, facilitate exercise and potentially improve the patient’s comfort. However, the relatively small risk of complications associated with right heart catheterisation should be discussed with the patient so they are able to give their informed consent to the procedure. The safety profile of non-invasive exercise stress testing is beyond the scope of this review. 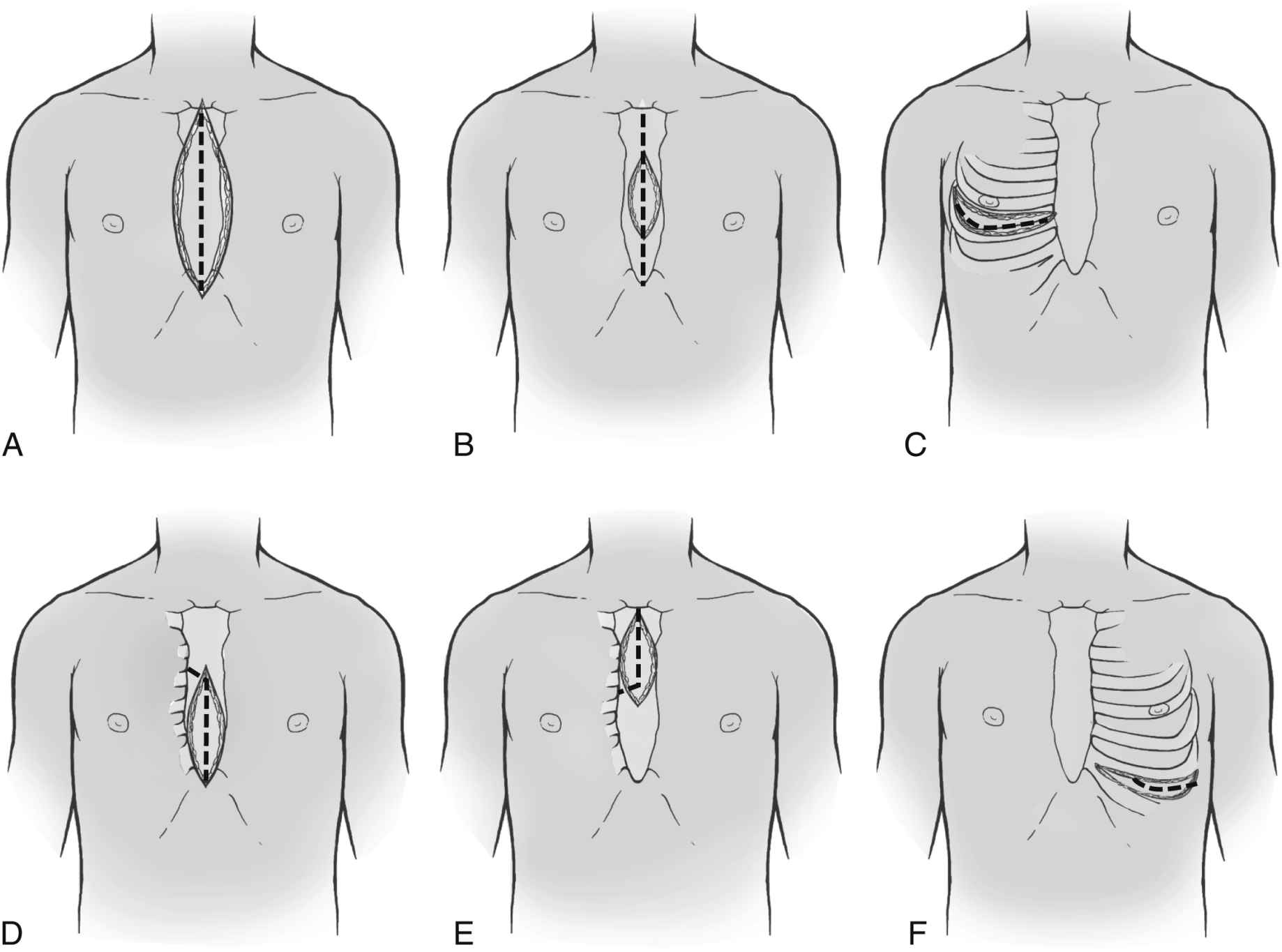
OXFORD HANDBOOK OF CARDIOTHORACIC SURGERY PROCEDURES HOW TOHow to Perform Exercise Right Heart CatheterisationĮxercise right heart catheterisation is more ergonomic when upper body venous access is used to place a multi-lumen pulmonary artery catheter which allows the lower body to be tested using a cycle ergometer. It will then address the implications of exercise right heart catheterisation to improve diagnosis and treatment in valvular heart diseases. It will address methodological considerations of exercise right heart catheterisation before discussing ‘normal’ invasive cardiopulmonary responses during exercise – an important contextual framework required for identifying and understanding pathophysiological abnormalities. The objective of this review is to discuss the diagnostic contribution of exercise right heart catheterisation in cardiovascular disease. Haemodynamic response patterns to exercise may also assist in assessing the severity of valvular heart disease, which can help to improve the management of these conditions. The differentiation of these two pathophenotypes is a key element of exercise right heart catheterisation. Exercise right heart catheterisation provides an opportunity to identify haemodynamic phenotypes that reflect a reduction in pulmonary vascular and/or cardiac function, which may not be evident when the patient is at rest. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
